Improving bone health prior to joint replacement surgery.

The importance of osteoporosis to joint replacement surgery.
Total hip arthroplasty (THA) and total knee arthroplasty (TKA) are among the most commonly performed orthopedic procedures. Osteoporosis has been identified as a risk factor that affects the success outcomes of total joint arthroplasty (TJA). Complications associated with TJA include intraoperative fracture, aseptic loosening of the prosthesis, and periprosthetic fracture. Studies have shown that osteoporosis increases the incidence of periprosthetic fractures by 0.3–5.5% after primary joint replacement surgery, and up to 30% following revision joint replacement surgery.
Studies on the incidence of osteoporosis in patients undergoing TJA have reported that 36.7% of patients who undergo joint replacement surgery have osteoporosis. Furthermore, patients who have undergone TJA are at an increased risk of developing osteoporosis after surgery due to postoperative bone loss. Research has found that bone mass loss around the operated joint can increase by up to 20% following TJA
Osteoporosis Medications and Their Outcomes in Improving Bone Health
Evidence suggests that the use of antiresorptive agents can reduce postoperative bone loss following total joint arthroplasty (TJA). A study by Ro et al. found that patients receiving bisphosphonates had a lower rate of revision total knee arthroplasty (TKA) compared with patients who did not receive pharmacological treatment (1.5% vs. 2.9%).
Similarly, studies in patients undergoing total hip arthroplasty (THA) demonstrated that those treated with bisphosphonates had a lower rate of revision THA compared with patients who did not receive medication (2.8% vs. 5.3%).
Furthermore, a meta-analysis has shown that the administration of bisphosphonates can reduce the risk of revision TJA by up to 50%.
Guidelines for the Evaluation and Treatment of Osteoporosis Before TJA Surgery
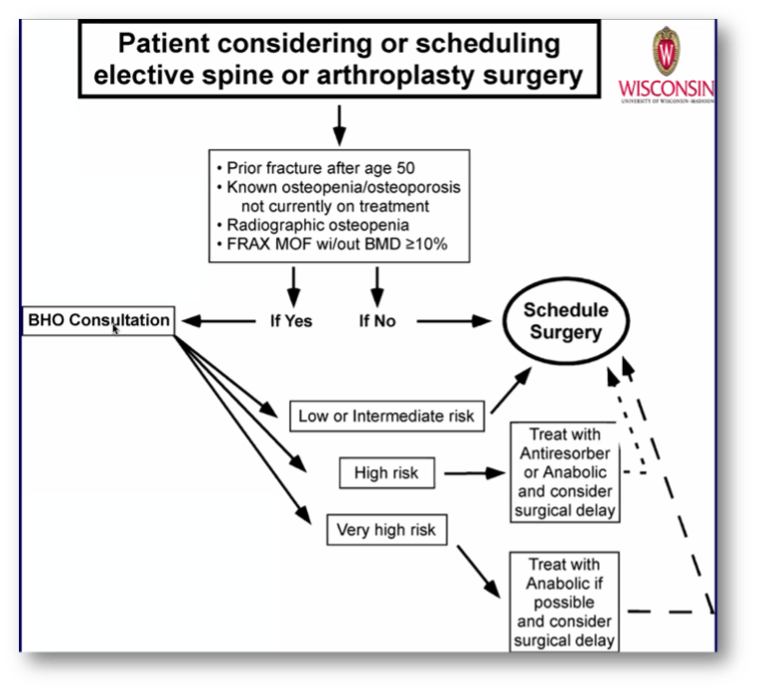
Summary
Osteoporosis is a common condition, particularly among patients who are scheduled to undergo Total Joint Arthroplasty (TJA). However, most patients receive very limited screening, risk assessment, and treatment for osteoporosis prior to TJA. The coexistence of osteoporosis with osteoarthritis can lead to poorer postoperative outcomes, such as intraoperative fractures, aseptic loosening of the prosthesis, and periprosthetic fractures.
Pharmacological treatment, including both anti-resorptive agents and anabolic bone-forming agents, has been shown to improve radiographic and clinical outcomes. Therefore, evaluation and optimization of bone health using osteoporosis medications should begin approximately 2–6 months prior to TJA and should be continued for at least 1–2 years after surgery. This approach can help improve treatment outcomes and reduce the risk of postoperative complications.
Source : Doctorwat
**Translated and compiled by ArokaGO Content Team
Police General Hospital
Share this article
More Articles
Discover more insights on health care and medical tourism.

Songkran Warning: How to Prevent and Handle “Shoe Suction” Injuries During Water Festival Celebrations
As Thailand celebrates Songkran, many festival-goers are enjoying water splashing in the streets, but one surprisingly common issue keeps returning every year, the so-called “shoe suction” problem, when wet slip-on sandals or rubber shoes become stuck tightly to the foot or ankle after prolonged exposure to water.

Office Syndrome: A Common Health Problem Among Modern Workers
In an era when working in front of a computer has become part of everyday life, Office Syndrome has emerged as one of the most common health concerns among working-age adults.

Urine does not flow, cannot hold urine
Urine does not flow, cannot hold urine, check urgently before it becomes an enlarged prostate or BPH (Benign Prostate Hyperplasia).